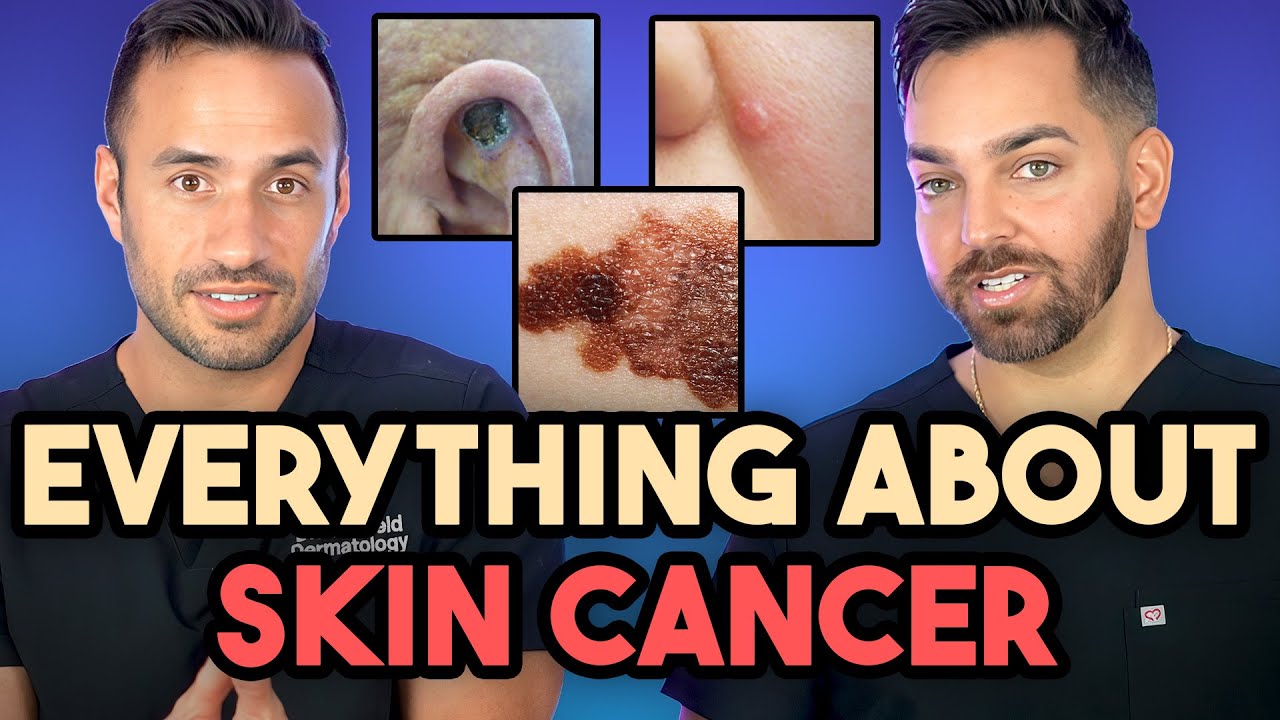
Most melanomas found in private practice detected on full-body screen, not by patients
Reuters Health • The Doctor's Channel Daily Newscast
The results also indicate that when the melanoma is first detected by a dermatologist, it is thinner and more likely to be in situ than when it is first found by the patient.
Prior to the study, the most recent update on skin cancer screening from the U.S. Preventive Services Task Force called the current evidence “insufficient to assess the balance of benefits and harms of screening for skin cancer by primary care clinicians of by patient skin self-examination,” study co-authors Deborah Kantor and Dr. Jonathan Kantor, from North Florida Dermatology Associates, Jacksonville, comment in the Archives of Dermatology for August.
However, “These data suggest that minimizing the substantial public health and financial impact of melanoma may be aided by a FBSE,” they note.
Their study featured 126 patients with melanoma who were seen at a private dermatology practice from July 2005 to October 2008. Of the melanomas, 51 were invasive and 75 were in situ.
A dermatologist detected 56.3% of the melanomas, while the remainder were identified by the patients, the authors note.
The bulk of melanomas in situ—60%–were detected by the dermatologist, the report indicates.
Moreover, the median depth of physician-detected tumors was 0.33 mm, much thinner than the median 0.55 mm-depth seen with patient-detected tumors. Dermatologist detected melanomas were five times more likely to be less than 1 mm than were those found by the patient.
The current findings, while supportive of FBSE screening for skin cancer, are not definitive, Dr. Daniel G. Federman, from VA Connecticut Health Care, West Haven, and colleagues note in a related editorial. “Although ‘more research is needed’ is an overused statement,” they add, “the claim does apply to the current situation.”
Reference:
Arch Derm 2009;145:873-876,926-927.